Wayne Lowry
Continuity of care in DPC plays a crucial role in transforming the patient experience. Unlike traditional healthcare models, Direct Primary Care builds and nurtures ongoing relationships between patients and their physicians, ensuring consistent and personalized attention. This approach helps patients feel truly heard and understood, leading to better health outcomes.
For those seeking a more connected and accessible healthcare experience, continuity of care in DPC offers unmatched benefits. Patients enjoy longer visits, direct communication with their doctors, and care tailored specifically to their needs. This patient-centered model reduces frustration and confusion, making healthcare simpler and more effective.
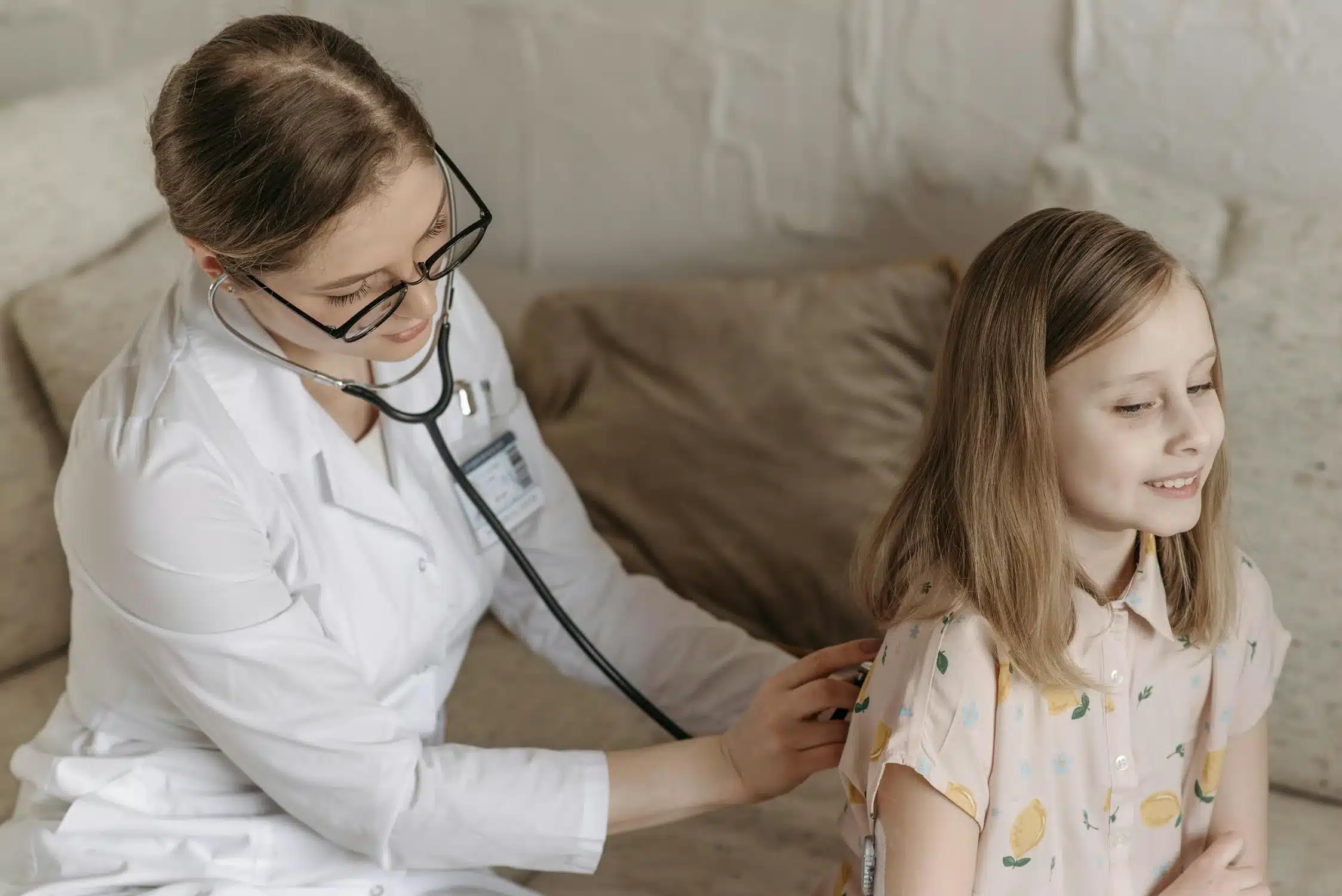
Continuity of care in Direct Primary Care (DPC) forms the foundation for personalized, patient-centered healthcare. It strengthens the doctor-patient relationship by ensuring ongoing medical attention tailored to individual needs.
Continuity of care describes the ongoing, consistent partnership between a patient and their healthcare provider. It involves detailed knowledge of the patient’s history, coordinated management of chronic conditions, and timely preventive care—all contributing to better health outcomes. This long-term collaboration reduces care fragmentation, lowers emergency department visits, and enhances patient satisfaction. Continuity supports cost transparency and efficient use of resources, making it a critical aspect of affordable healthcare and comprehensive services.
Direct Primary Care (DPC) operates on a subscription model where patients pay a fixed monthly fee directly to their primary care physician. This subscription covers comprehensive services such as annual check-ups, preventive care, chronic disease management, and specialist referrals without traditional insurance barriers.
The DPC model prioritizes direct access and longer visits, allowing physicians to focus on personalized medicine and holistic approaches.
As it eliminates insurance claims, copays, and deductibles, DPC promotes clear cost transparency and supports effective care coordination. This model empowers healthcare providers to deliver attentive, flexible care that traditional systems often limit.
For more information on finding trusted DPC providers, visit Best DPC.

Continuity of care within the Direct Primary Care (DPC) model strengthens the doctor-patient relationship, improves health outcomes, and supports cost-effective access to healthcare. These benefits arise from the subscription model’s focus on personalized medicine and comprehensive services.
Consistent access to the same primary care physician deepens trust and exploring between patients and healthcare providers. The DPC model encourages longer visits—typically lasting 30 to 60 minutes—which provide time for thorough discussions and personalized care planning. This approach promotes a holistic view of health, allowing physicians to consider lifestyle, environment, and patient preferences.
Direct access to providers, including same-day appointments and 24/7 communication options, removes typical barriers in traditional care, such as restricted office hours and rushed encounters. This leads to higher patient satisfaction and stronger engagement in preventive care and chronic disease management. Consistent doctor-patient relationships further reduce care fragmentation through better care coordination and more accurate tracking of specialist referrals.
Continuity in DPC supports proactive health management by enabling physicians to monitor patient history comprehensively over time. This ongoing partnership facilitates timely preventive care and more effective chronic disease management, such as diabetes or hypertension control. The reduction of emergency department visits and hospital admissions correlates with continuous patient oversight.
Physicians operating within the DPC model can provide personalized medicine free from insurance constraints, allowing for tailored treatment plans that respond directly to patient needs. Comprehensive services within the subscription model ensure that care remains patient-centered, enhancing compliance and reducing complications. This ultimately contributes to better clinical outcomes and improved overall wellbeing.

The subscription model of DPC offers transparent, predictable pricing through flat monthly fees, eliminating copays, deductibles, and surprise bills typical in insurance-based systems. This encourages patients to seek care early without fear of unexpected costs, increasing access to care for routine and preventive services.
Self-pay options and discounted services within DPC practices reduce administrative complexity and overhead, benefiting both patients and providers. Moreover, employers and patients experience fewer sick days and increased productivity due to healthier populations supported by continuous, coordinated care.
Although DPC focuses on primary care, its comprehensive services—ranging from annual check-ups to chronic disease management—deliver affordable healthcare that emphasizes prevention and long-term health maintenance.
Direct Primary Care (DPC) strengthens continuity of care by ensuring patients benefit from ongoing, personalized medical relationships. This model removes common barriers found in traditional healthcare, enhancing access and patient engagement.
DPC emphasizes personalized medicine through extended visits and direct access to the primary care physician. Typical appointments last 30 to 60 minutes, allowing providers to address chronic disease management, preventive care, and holistic health concerns without feeling rushed. Patients experience streamlined communication via phone or telehealth, often with same-day or next-day scheduling.
This accessibility fosters a strong doctor-patient relationship, essential for early diagnosis and tailored treatment plans. Eliminating insurance claims and copays simplifies cost transparency and encourages patients to seek care proactively, supporting better health outcomes.
Smaller patient panels and a subscription model relieve physicians from administrative burdens common in traditional systems. This reduction in bureaucracy lowers provider burnout and supports continuity by enabling doctors to focus entirely on patient-centered care. Patients see the same healthcare provider consistently, which reduces turnover and creates a trusting environment. For providers, this model revives the passion for medicine while enhancing job satisfaction. The stability from monthly fees allows healthcare providers to maintain longer appointments and comprehensive services, reinforcing a sustainable care partnership.

DPC practices integrate care coordination to manage chronic conditions and specialist referrals effectively. Dedicated teams work alongside the primary care physician to monitor treatments, follow hospital admissions, and ensure continuity across healthcare settings. This coordinated approach reduces care fragmentation and hospital readmissions. Although DPC focuses on primary care, transparent service agreements clarify specialist referrals and supplemental insurance needs. The holistic approach includes annual check-ups and preventive care, empowering patients to maintain long-term health with comprehensive oversight.
Continuity of care in Direct Primary Care helps shape healthcare experience that’s both personalized and efficient. By fostering strong patient-provider relationships, DPC empowers patients to take an active role in their health while enabling physicians to deliver comprehensive, coordinated care.
This model’s emphasis on accessibility, longer visits, and transparent pricing creates an environment where prevention and chronic disease management thrive. While challenges exist, ongoing innovations and integrations continue to enhance DPC’s ability to provide consistent, high-quality care.
For anyone seeking a healthcare approach centered on trust, engagement, and improved outcomes, DPC offers a compelling alternative to traditional models.
Direct Primary Care is a healthcare model where patients pay a fixed monthly fee directly to their primary care physician. It offers comprehensive services without traditional insurance barriers, focusing on longer visits, personalized care, and direct communication.
Continuity of care builds ongoing relationships between patients and physicians, allowing better understanding of medical history, coordinated chronic disease management, and preventive care, resulting in improved health outcomes and patient satisfaction.
Longer visits allow physicians to spend more time addressing patient concerns, discussing preventive care, and managing chronic conditions, leading to personalized and thorough care that improves overall health management.
DPC removes insurance hassles like copays and deductibles, offers direct communication with physicians, and provides clear, transparent pricing, simplifying the healthcare process and reducing patient frustration.
Yes, challenges include limited scope since patients still need insurance for specialists and emergencies, affordability for low-income patients, and potential difficulties for doctors starting DPC practices due to income and support issues.
Integrating DPC with Medicaid or employer-sponsored plans can improve affordability and access, ensuring more people benefit from personalized care without financial strain.
Yes, smaller patient panels and more patient-centered care reduce physician stress and burnout, improving job satisfaction and enabling better care delivery.
Ongoing care relationships in DPC reduce care fragmentation, leading to fewer emergency visits by managing conditions proactively and providing timely preventive services.
Absolutely, DPC emphasizes clear communication and personalized approaches, which help engage diverse populations effectively for better health outcomes.
Best DPC offers a reliable network of patient-centered physicians committed to affordability, coordination, and comprehensive personalized care. Their blog also provides useful insights and tips on navigating DPC.

ABOUT AUTHOR
Wayne Lowry
Wayne Lowry, Founder of BestDPC, is a passionate advocate for Direct Primary Care (DPC) and its mission to deliver personalized, accessible healthcare. He believes that DPC providers should serve as the trusted first point of contact for all medical needs, ensuring patients never feel isolated or uncertain about their health decisions. Through his work, he champions a patient-first approach to healthcare, building a system that prioritizes guidance, support, and trust.

Thank You for Registering!
Your registration was successful! We're excited to have you on board. Please check your email for a confirmation link to complete your registration.